People think that because diabetes is a disease marked by high levels of blood sugar, eating sugar is a problem. On the surface it makes sense. But that’s not how it works. A healthy person can eat as much sugar, as much carbohydrate, as they want and as long as their cells take it up, they won’t have high blood sugar. The problem occurs when cells resist taking up glucose from the bloodstream. (Which has several causes which I’ve discussed over the years.)
I’m noticing a similar mindset with sarcopenia, a disease marked by loss of muscle mass as we age. People think that because muscles contain protein, eating more protein can preserve muscle. On the surface it makes sense. But that’s not how it works. In fact, it can backfire and cause even greater loss of muscle. (Because a high-protein diet contributes to acidosis. See below.*)
Here’s something I wrote a few years ago:
________
Up To A Third Of Adults Over 50 Have Some Degree Of Muscle Loss (Sarcopenia), More Protein Doesn’t Seem To Help
The following study looked at 9 placebo-controlled studies (the gold standard of scientific investigation), and found no benefit from protein:
Clinical Effectiveness Of Protein And Amino Acid Supplementation On Building Muscle Mass In Elderly People: A Meta-Analysis, PLOS ONE, 30 September 2014
Conclusions: These results indicate that amino acid/protein supplements did not increase lean body mass gain and muscle strength significantly more than placebo in a diverse elderly population.
This next one was an exhaustive review of 37 studies from January 2000 to October 2013 that addressed the prevalence of sarcopenia and the effect of nutrition and exercise.
Prevalence Of And Interventions For Sarcopenia In Ageing Adults: A Systematic Review. Report Of The International Sarcopenia Initiative (EWGSOP and IWGS), Age and Aging, 21 September 2014
In a nut shell:
- Up to a third (33%) of adults over 50 (living in the community, not in a care setting where, as you’d expect, the prevalence is higher) have some degree of muscle loss or reduced muscle function.
- “Protein supplements have not shown consistent benefits on muscle mass and function.”
- “Exercise interventions, especially those based on resistance training, may have a role in improving muscle strength and physical performance (moderate quality evidence), but not muscle mass.”
________
Not only can eating too much protein contribute to muscle loss, it also stresses the kidney. As we saw, excess protein increases calcium losses, and increases risks for kidney stones and renal disease.
Related: High-Fat Diets Contribute To Age-Related Muscle Loss (Sarcopenia)
* How eating too much protein can backfire:1,2
While consuming an adequate amount of protein is important for older adults, consuming too much protein can result in a low-level, diet-induced metabolic acidosis, or abnormally increased acidity in the body. The typical American diet—which is high in animal proteins and cereal grains, and low in fruits and vegetables—can cause a low-grade metabolic acidosis that contributes to the decline in muscle and bone mass found in aging adults.
1 Life Extension, Preventing Sarcopenia, January 2007
2 Diet, Evolution And Aging – The Pathophysiologic Effects Of The Post-Agricultural Inversion Of The Potassium-To-Sodium And Base-To-Chloride Ratios In The Human Diet, European Journal of Nutrition, October, 2001

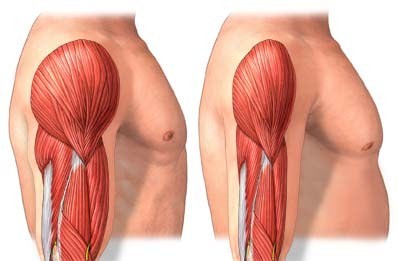
Note that while exercise was shown to improve muscle strength and performance, it did not increase muscle mass.
LikeLike
Pingback: Sarcopenia. It’s complex. | Fanatic Cook
Pingback: To Preserve Muscle: Eat Regular Meals. No Fasting. | Fanatic Cook